CHIAs Project — Scaling up community action to find people missing from tuberculosis care
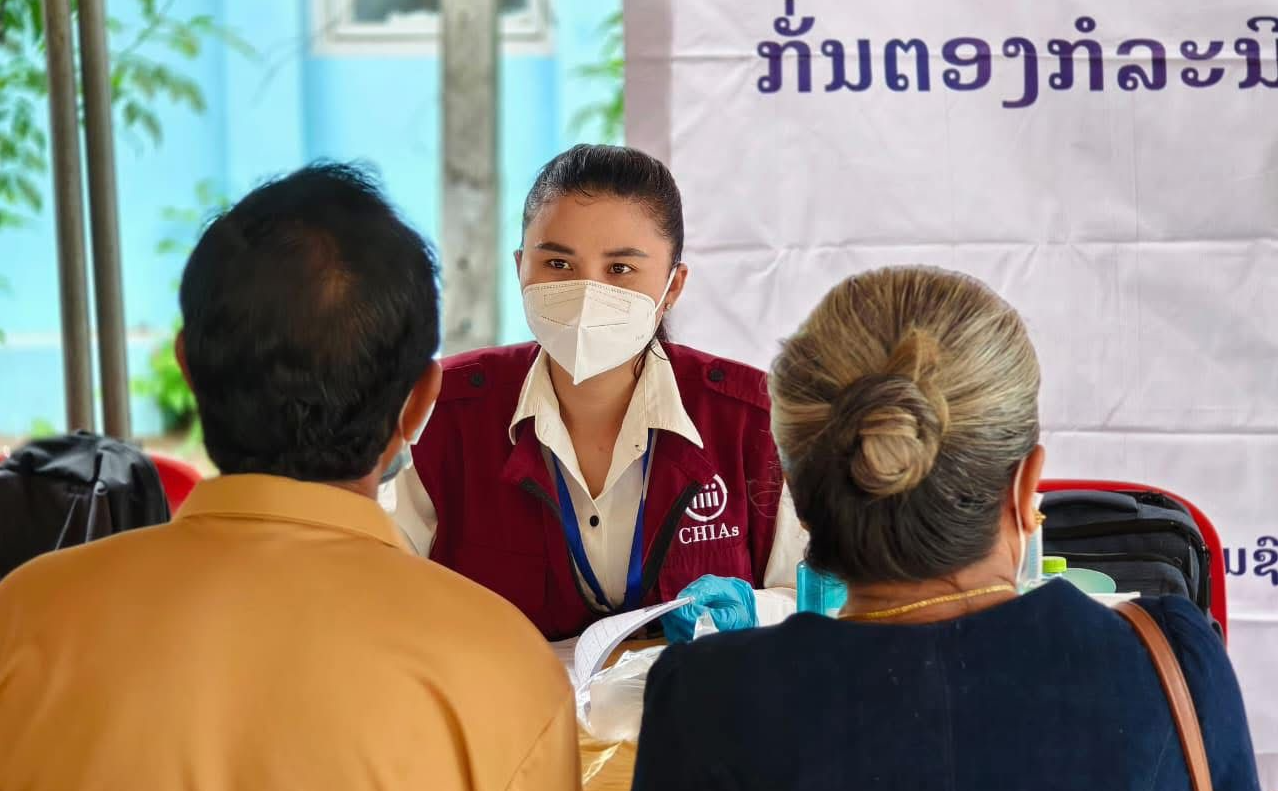
Building on work in Bolikhamxay and Khammouane, CHIAs Phase 2 focuses on Savannakhet, in Laos: decentralized active case finding, stronger specimen transport, and a step-up on pediatric preventive treatment (TPT). Mr. Viengakhone Souriyo explains how community volunteers, mobile logistics and clinic partnerships close gaps between remote villages and care.
What is CHIAs Phase 2 and how does it build on earlier lessons?
Viengakhone SOURIYO: CHIAs Phase 2 accelerates tuberculosis (TB) elimination in Savannakhet by scaling active case finding and strengthening community-led systems. From Phase 1 we learned that trust and local ownership matter: Phase 2 decentralizes detection with village volunteers equipped with digital referral tools, intensifies pediatric screening and embeds TPT for child contacts. Empowering TB survivors and village leaders ensures adherence support and a sustainable bridge between remote communities and district services.
Which concrete results from Phase 1 shape Phase 2 — and what early gains do you see?
Viengakhone SOURIYO: Phase 1 screened 6,938 high-risk people and detected 798 active TB cases — a 95% increase in notifications — with all confirmed patients started on treatment. In Phase 2 we target broader contact investigation and pediatric TPT: we aim to screen more than 100 household contacts and start 50 children on TPT. Early signs are promising: community referrals rose 62%, and over 620 TB cases were identified through the decentralized approach, proving that village volunteers find presumptive cases faster than passive facility-based detection.
How do you solve logistics — specimen transport, seasonality and mobile units?
Viengakhone SOURIYO: Distance and poor roads are major barriers. We created a specimen transport network using trained volunteers and motorbikes to deliver sputum to district laboratories within 24 hours. During the rainy season, we preposition supplies and schedule mobile campaigns during dry periods or around village events. Where provincial laboratories are distant, GeneXpert at the district level provides rapid, on-site confirmation and reduces referral delays.
How do you detect and keep children on TPT — and how do communities and clinics collaborate?
Viengakhone SOURIYO: Passive case finding at health facilities misses most pediatric TB. We therefore conduct active household contact investigations: volunteers screen child contacts at home and refer them for clinical assessment. Health centre staff are trained on pediatric TPT protocols; volunteers monitor adherence and side effects and support medicine refills during routine visits. Clinicians handle diagnosis and prescriptions, while community actors ensure retention by addressing fears and transport or food barriers at the household level.
What evidence and evaluations will influence national policy?
Viengakhone SOURIYO: Building on Phase 1’s Monitoring & Evaluation and DHIS2 (District Health Information Software 2) recommendations, Phase 2 runs operational studies on diagnostic delays, cost per case and the added value of active case finding led by civil society organizations. We will present the findings to the National TB Program through technical working groups to advocate for scalable, community-based models and inform donor decisions.