World Malaria Day 2023
Africa continues to be the world’s most malaria-affected continent. In 2020, 95% of malaria cases and 96% of malaria deaths were reported by the World Health Organization (WHO) to have occurred in this region of the world. Yet funding is dropping off, and malaria-affected countries’ healthcare systems, already strained by the three-year struggle against COVID-19, are being undermined by the emergence of resistance to treatments and insecticides. In response to an upsurge in malaria, efforts to control the disease continue. L’Initiative is working with stakeholders in more than 40 countries.
The appearance in Africa of the Anopheles stephensi mosquito species is, therefore, worrisome to specialists. This malaria vector, native to Southeast Asia, is resistant to conventional insecticides and, unlike African anopheles, is particularly well adapted to the urban environment. A 2020 model suggests the species could threaten up to 126 million people in Africa were it to spread to the continent’s major cities.
Combating malaria at every level
These obstacles are all preventing the international community from reaching the WHO target of reducing malaria case incidence and mortality rates by at least 90% between 2015 and 2030.
Alongside the Global Fund and its country partners, Expertise France, through L’Initiative, provides technical assistance and innovation support in partner countries to increase the impact of programs financed by the Global Fund. Supported by research institutes, local NGOs, and governmental institutions, these programs apply prevention tools and strategies recommended by the WHO to control the disease: distribution of long-lasting insecticidal nets and/or indoor residual spraying for vector control, rapid access to diagnostic tests in case of suspected malaria, and treatment of confirmed cases with antimalarials.
Other projects supported by L’Initiative relate to WHO recommendations for vulnerable population groups, including intermittent preventive treatment for pregnant women and infants. Malaria affects pregnant women and under-fives most severely due to their weak immune systems, with a child dying from malaria every two minutes in the world, mostly in Africa. Finally, seasonal malaria chemoprevention, which has been recommended for the past ten years, has been shown to be effective, inexpensive, safe, and practicable for the prevention of malaria in children under five years of age in areas of high seasonal malaria transmission.

Seasonal mobile workers and malaria in Ethiopia
In Ethiopia, itinerant seasonal workers, although particularly exposed to malaria, are not taken into account in actions to combat the disease. The Ethiopian organization Health, Development and Anti-Malaria Association (HDAMA) and Malaria Consortium designed a project to meet the needs of these workers.

Community health workers in the Greater Mekong subregion
Despite a clear decrease in the incidence of malaria between 2012 and 2015, the parasite has developed resistance. Financed by a grant from the Global Fund of which L’Initiative is a partner, the Regional Initiative against Artemisinin Resistance (RAI) relies on a network of approximately 40,000 community health workers to fight against this drug resistance in villages and rural and forest areas of the region.
The importance of malaria research
Research is also progressing. The WHO recently announced that it is recommending a vaccine for children at risk of malaria. The RTS,S vaccine is currently being rolled out in three sub-Saharan African countries. However, financial support is needed to meet the public health challenges of strengthening health systems in high-incidence countries and of engaging communities to support vulnerable population groups. Without this support, all these tools can only have a limited impact.
Also, as the malaria parasite evolves and drug resistance rises, other approaches and new tools need to be developed. L’Initiative, therefore, remains committed to operational research and, since 2018, has put out a specific annual call for projects in order to support researchers. Operational research is key to ending major pandemics. Among other benefits, it tests innovative approaches to prevention, screening, and care and helps to develop more effective response strategies.

L’Initiative and operational research on malaria
Faced with the challenges posed by the evolution of the parasite and the increase in drug resistance, new tools and methods must be put in place. By evaluating new interventions in the pandemic response, operations research programs produce data that encourages scale-up.
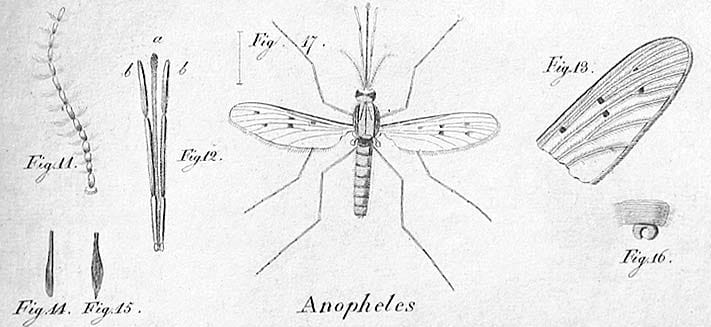
A new malaria vector in Africa: Anophele stephensi
L’Anophele stephensi is gaining ground in Africa. This species, previously never seen on this continent, carries the two most deadly strains of the parasites responsible for malaria. It appeared in the Horn of Africa in 2012 in Djibouti, when the country was preparing to eradicate the disease. Since then, Anophele stephensi has been spotted in Ethiopia, Sudan, Somalia, Nigeria and Kenya.