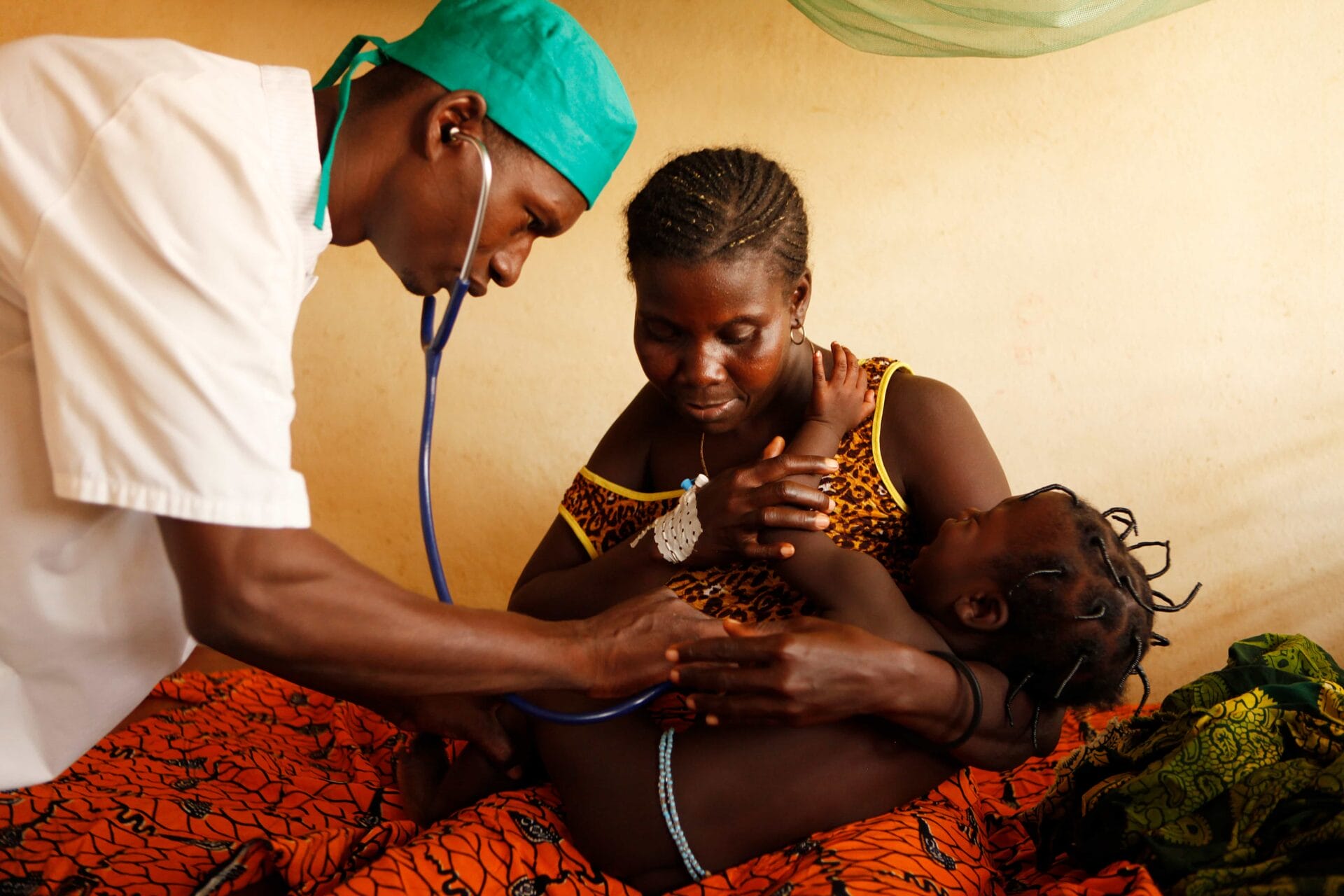
The fight to eliminate malaria in the Greater Mekong region is fraught with challenges, most notably that of the disease’s drug resistance. Since 2014, the Regional Artemisinin-resistance Initiative (RAI) has been helping to contain this Southeast Asian endemic. Since its launch, this grant represents over 60 million malaria screenings and 2.6 million patients treated for this deadly disease.
To combat malaria, a potentially fatal disease caused by parasites of the Plasmodium family and transmitted by the bites of anopheles mosquitoes, one of the leading treatments is a combinatorial therapy involving the use of artemisinin molecules. This therapy has been widely deployed, notably in the endemic Greater Mekong region (Cambodia, Laos, Myanmar, Thailand and Vietnam) in Southeast Asia. In 2013, however, studies revealed parasite resistance to the artemisinin molecule, raising the global issue of drug resistance in malaria. It was in this context that the Regional Artemisinin-resistance Initiative (RAI) in the Greater Mekong was created in 2013. This grant is funded by the Global Fund and the Initiative. In 2024, a fourth phase will run until 2026. In total, between 2014 and 2026, the RAI represents an investment of 650 million euros.
A fourth phase of the grant to eliminate malaria
The fourth phase of the RAI grant will concentrate efforts on eliminating the danger of malaria in the Greater Mekong region, focusing on at-risk and vulnerable populations (communities living in remote areas, migrant workers, ethnic minority populations). As all countries in the Greater Mekong region face similar challenges – migration, ethnic minority issues, difficult-to-access areas – they can benefit from similar solutions thanks to the RAI grant. RAI coordinates the surveillance of malaria cases, including those crossing borders, and ensures that all countries follow the recommendations. A set of actions made possible thanks to a solid network of partners, including the WHO regional office in Phnom Penh, brought together under the RAI leadership, and a coordination platform of civil society organizations in the region.
RAI also relies on a vast network of around 34,000 volunteers in the many communities living in the Greater Mekong, enabling a quick answer in case of epidemic resurgence via a screening and treatment directly administrated in the villages concerned. Malaria cases are detected and reported from a smartphone, feeding a national database in real time. Long-lasting insecticide-treated mosquito nets have been distributed to over 33 million households throughout the Greater Mekong region. “We are close to achieving our malaria elimination targets in all five countries. RAI has enabled us to fight malaria effectively in a wide variety of contexts, including migrant populations, ethnic minorities and forest areas. And we have improved the level of epidemiological surveillance,” explains Izaskun Gaviria, the Global Fund Portfolio Manager. “The projects funded have been essential in reducing the prevalence of malaria, against a backdrop of increasing resistance to treatment, making elimination of the disease a matter of urgency. It is vital to maintain the level of funding to ensure the continuity of mapping, prevention, screening and treatment activities, at community level and in all the areas concerned. The availability of effective treatments against multi-drug resistant strains will be essential if we are to achieve the goal of eliminating malaria from the region”, adds Arjen Dondorp, Chairman of RAI’s Regional Coordinating Body.


The Regional Artemisinin-resistance Initiative (RAI) aims to stem the malaria epidemic in Southeast Asia, focusing on combating the emergence of antibiotic resistance phenomena in particular.
RAI monitors the evolution of malaria cases and ensures that all players in the Greater Mekong region follow health recommendations. “This is made possible by a strong network of local partners, including civil society organizations. Over the course of the three funding campaigns launched since 2013, L’Initiative has provided RAI with the resources needed to recruit high-level consultants to support RAI’s grant applications, at both national and regional levels,” completes Izaskun Gaviria.